Abstract
Introduction: The 17p deletion (del(17p)) resulting in loss of the TP53 gene is associated with impaired response to genotoxic agents and has an impact on PFS following BTK inhibitor and possibly also venetoclax. The del(17p) usually coincides with TP53 mutation, leading to the impairment of the p53-associated pathway. Sole TP53 mutations appear also associated with poor outcome in prospective trials. The iwCLL guidelines recommend to look for del(17p) and TP53 mutation before each line of treatment. An original approach is the functional assay, which highlights the functional abnormalities of p53 whether it is a TP53 gene disruption (del(17p) and/or TP53 mutation) or a defect of another actor in the p53 pathway. We aim to validate this functional assay on a prospective trial and to study the impact of p53 status on the clinical response regardless of the biological method.
Methods: Clinical and biological data were collected from 74 CLL patients (pts) enrolled in the BOMP phase II trial of the French Innovative Leukemia Organization (FILO) (NCT01612988) evaluating 6 monthly courses of BOMP including bendamustine, ofatumumab and high dose methylprednisolone in fit pts with relapsing CLL. In addition to conventional screening, we focused on p53 evaluation at time of inclusion. FISH analysis for del(17p) was done with a 5% cut-off for positive result. TP53 gene mutation screening was performed by Sanger sequencing of the coding region (exons 2-11). A targeted NGS screening (19 genes including TP53, Illumina MiSeq) was also performed. The p53 functional status was determined by a flow cytometry assay based on induction of p53 and p21 protein expression after etoposide and nutlin-3 exposition, as previously described (Le Garff-Tavernier M., 2011), which allows the detection of 3 types of p53 dysfunction (A, B and C), irrespective of an ATM default. Clinical response was evaluated by PFS, OS and TTNT Kaplan-Meier analyses (MedCalc stat).
Results: Data from the whole cohort are available. Median age was 64 yrs. Pts had a median of 1 (1-3) lines of treatment previous to this trial, including FCR in >90%. Concerning p53 evaluation, a del(17p) was found in 30% of cases by FISH (22/73 pts with a median of 68% positive cells, range 10-98). The percentage of p53 abnormalities increased to 41% when TP53 mutations were screened (30/73 pts with 1 to 8 mutations, median VAF 10 %, range 1.6-90). Results from the p53 functional assay were available for 69 pts showing the highest level of p53 abnormalities. Indeed, p53 dysfunction was observed in 48% of pts (33/69) including type A (n=11), type B (n=17) and type C (n=5) dysfunction.
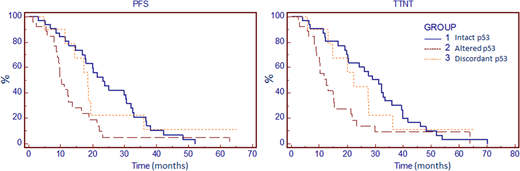
Thus, the sensitivity and specificity of the p53 functional assay to detect pts with del(17p) and/or TP53 mutation were of 87% and 84% respectively (n=68 pts for which the 3 tests were available). Interestingly, discordant results were observed in 10 pts: 4 pts with a functional p53 despite a TP53 gene disruption (3 with TP53 mutation only and 1 with del(17p) only) and conversely 6 pts with a p53 dysfunction (all with type B dysfunction) but without any TP53 gene disruption, suggesting alternative alterations of the p53 pathway. The only similarity for those latter pts is the occurrence of at least one ATM abnormality (del(11q) and/or ATM mutation). The combination of the 3 assays defines 3 groups: (1) "intact p53" (no TP53 disruption and functional p53, n=32), (2) "altered p53" (TP53 disruption and p53 dysfunction, n=26) and (3) "discordant p53" (n=10).
PFS and TTNT were higher in pts without (n=38) compared to those with TP53 gene disruption (n=30) (p=0.04 for both). The OS, even though not significant, presented a similar trend. When considering the functional status, a similar profile is observed but with a better discrimination between pts with normal p53 function (n=36) and pts with p53 dysfunction (n=32) (p=0.002 and 0.003, respectively). Combining the 3 assays, PFS and TTNT of the group 3 "discordant p53" profiles' appeared intermediate (Figure 1).
Conclusion: This study shows that a p53 functional analysis can predict with an acceptable sensitivity the presence of a TP53 gene disruption. Interestingly, this functional assay coupled with cytogenetic and mutational screening could reveal a sub-group of pts with discordant results for which PFS and TTNT appeared intermediate. Evaluation of other discordant cases is mandatory to confirm these results and could lead to a wider use of this global functional approach.
Feugier:Abbvie: Consultancy, Honoraria, Membership on an entity's Board of Directors or advisory committees, Research Funding; Janssen: Consultancy, Honoraria, Membership on an entity's Board of Directors or advisory committees, Research Funding; Roche: Consultancy, Honoraria, Membership on an entity's Board of Directors or advisory committees, Research Funding; Gilead: Consultancy, Honoraria, Membership on an entity's Board of Directors or advisory committees, Research Funding. Sylvain:Gilead: Other: scientific advisor board. Schuh:Giles, Roche, Janssen, AbbVie: Honoraria. Guieze:abbvie: Honoraria; janssen: Honoraria; gilead: Honoraria. Leblond:Abbvie: Consultancy, Honoraria, Other: Travel, Accommodations, Expenses, Speakers Bureau; Roche: Consultancy, Honoraria, Other: Travel, Accommodations, Expenses, Speakers Bureau; Janssen: Consultancy, Honoraria, Speakers Bureau; Gilead: Honoraria, Speakers Bureau; Sandoz: Honoraria; Amgen: Honoraria.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal